Is There a Cure for Epidermolysis Bullosa? Types, Treatments & Daily Care
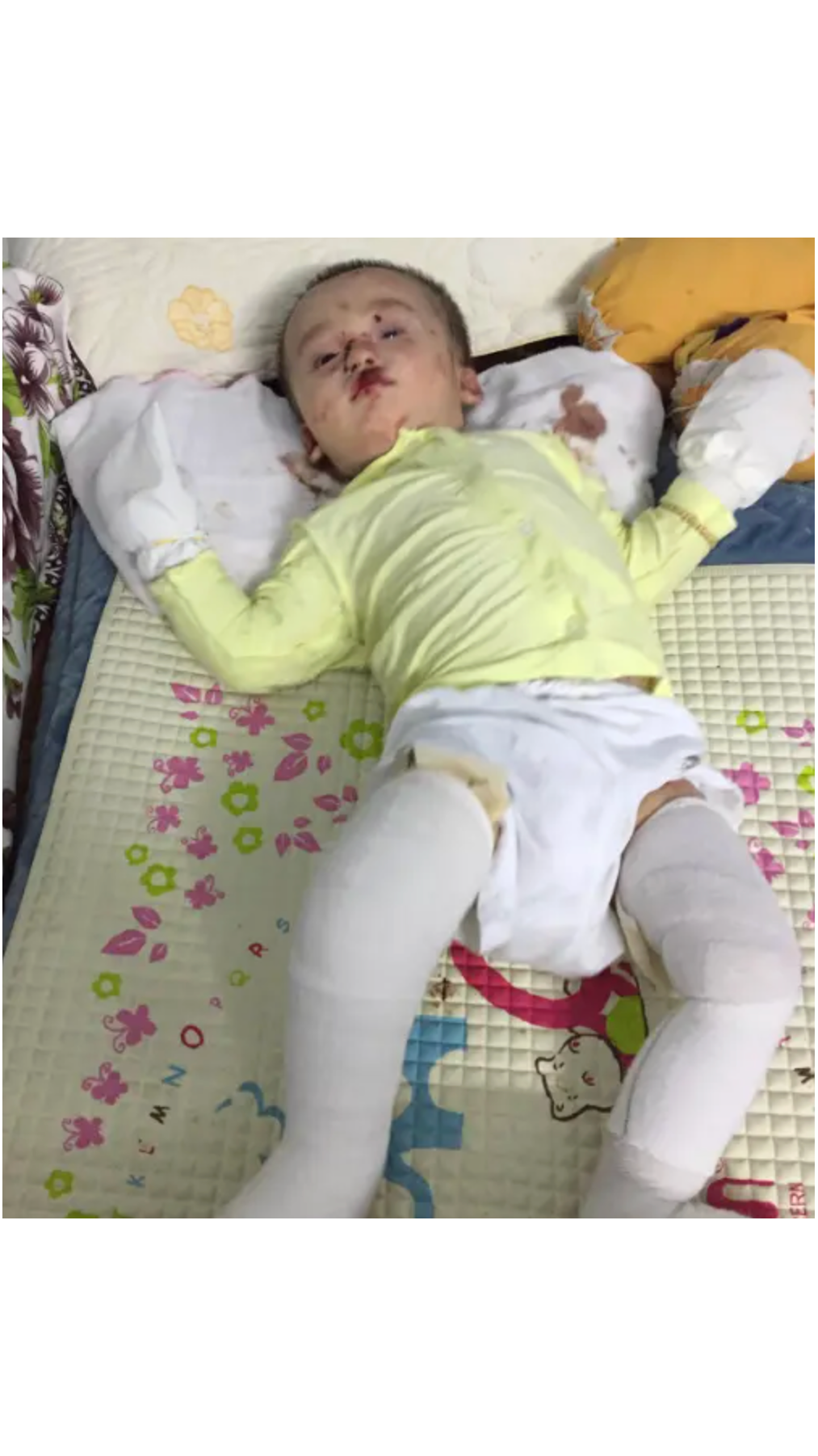
Receiving an EB diagnosis is the beginning of a steep learning curve. Understanding how the condition works, what complications to watch for, and which daily management strategies actually hold up in practice can make a measurable difference in long-term outcomes.
What Is Epidermolysis Bullosa ("Butterfly Skin")?
Epidermolysis Bullosa represents a group of rare, inherited genetic disorders that cause extreme skin fragility and painful blisters from even the gentlest touch. Often called "butterfly skin" because it's as delicate as a butterfly's wings, EB affects approximately 20 per million live births in the United States, with around 500,000 people currently living with various forms of the condition worldwide.
The condition stems from mutations in at least 16 different genes responsible for producing proteins that bind skin layers together. When these proteins are missing or defective, the skin literally separates and tears with minimal friction or trauma. Unlike other skin conditions, EB is not contagious and typically manifests from birth, though some milder forms may not become apparent until later in childhood or even adulthood.
Four Main Types Affect Different Skin Layers
Understanding which type of EB affects a child is vital for developing appropriate care strategies and setting realistic expectations for the future. Each type occurs at different layers within the skin structure and presents unique challenges for families.
1. EB Simplex (Most Common)
EB Simplex accounts for approximately 70% of all EB cases and typically represents the mildest form of the condition. Blistering occurs within the epidermis (outer skin layer) and primarily affects the hands and feet, especially areas subject to friction like palms and soles. Many children with EBS can participate in modified activities and may see some improvement as they age, though daily management remains necessary.
2. Dystrophic EB (Causes Scarring)
Affecting roughly 20-25% of EB patients, Dystrophic EB occurs deeper in the dermis layer and produces significant scarring as wounds heal. This scarring can gradually cause fingers and toes to fuse together, creating "mitten-like" hands and feet. Children with severe forms face increased risks of skin cancer, particularly aggressive squamous cell carcinoma that can develop in chronically wounded areas.
3. Junctional EB (Severe Forms)
Junctional EB represents approximately 5% of cases and affects the junction between the epidermis and dermis. This type frequently involves extensive blistering of mucous membranes, including the mouth, throat, esophagus, and even internal organs. Severe forms can be life-threatening, particularly in infancy.
4. Kindler EB (Mixed Features)
Kindler EB is often considered the rarest form and presents a unique combination of features from other types, often including photosensitivity (sensitivity to sunlight) along with the characteristic skin fragility. While less common, this type requires specialized sun protection strategies in addition to standard EB management approaches.
Serious Complications Parents Must Watch For
Beyond the daily challenge of managing fragile skin, EB can lead to several life-threatening complications that require immediate medical attention and long-term monitoring.
Infection and Sepsis Risks
Open wounds create constant entry points for bacteria, making infection a persistent threat. Signs of serious infection include increased redness around wounds, unusual warmth, foul-smelling drainage, fever, or changes in a child's energy level or appetite. Sepsis, a life-threatening response to infection, can develop rapidly in children with extensive open wounds and requires emergency medical intervention.
Nutritional Challenges from Oral Blistering
When EB affects the mouth, throat, and esophagus, eating becomes painful and potentially dangerous. Chronic blistering can lead to esophageal strictures (narrowing), making swallowing difficult or impossible. Many children require feeding tubes or specialized diets to prevent malnutrition and maintain healthy growth patterns.
Skin Cancer in Certain EB Types
Particularly concerning in Dystrophic EB, aggressive skin cancers can develop in areas of chronic wounding and scarring. These cancers tend to be more aggressive than typical skin cancers and require vigilant monitoring by dermatologists familiar with EB. Early detection and treatment are critical for the best outcomes.
Daily Wound Care Is Your Child's Lifeline
Effective wound care forms the foundation of EB management, requiring specialized techniques and supplies that differ significantly from standard first aid approaches.
Supplies Every EB Family Needs
Successful EB management requires maintaining a well-stocked supply of specialized materials:
- Non-adherent dressings that won't stick to fragile skin
- Sharp scissors for precise cutting and trimming (sanitized after each use)
- Retention bandages to secure dressings without adhesives
- Antimicrobial cleansers to reduce infection risk
- Moisturizers specifically designed for compromised skin
- Pain relief medications as prescribed by healthcare providers
Proper Blister Care Techniques
Unlike typical blisters that should remain intact, EB blisters require careful drainage to prevent them from enlarging and causing additional skin damage. Using a sterile needle or lancet, carefully puncture the blister at its edge and gently drain the fluid while leaving the "roof" of skin intact to protect the underlying wound. This technique requires practice and should initially be demonstrated by experienced healthcare providers.
Non-Adherent Dressing Guidelines
Traditional bandages and adhesive dressings can cause catastrophic skin damage when removed. Instead, use silicone-based or specially designed non-adherent dressings that can be changed without trauma. Layer these with soft retention bandages, ensuring they're snug enough to stay in place but not tight enough to restrict circulation or cause pressure sores.
Managing Chronic Pain and Discomfort
Pain management in EB often requires a multi-faceted approach combining prescription medications with topical treatments and comfort strategies.
Prescription Pain Management Options
Many children with EB require around-the-clock pain medication, particularly those with severe forms. Healthcare providers may prescribe everything from mild analgesics for daily management to stronger opioid medications for severe flare-ups or dressing changes. Working with pain management specialists familiar with EB can help optimize medication regimens while minimizing side effects and dependency concerns.
Topical Relief Strategies
Topical anesthetics applied before dressing changes can significantly reduce procedural pain. Cooling techniques, specialized moisturizers, and anti-itch medications help manage daily discomfort. Many families find that keeping the child's environment cool and using soft, natural fabrics like silk or bamboo reduces friction and irritation.
Promising Gene Therapy Research Offers Hope
Recent breakthroughs in EB research are providing unprecedented hope for families facing this challenging condition. The FDA has approved Vyjuvek, a topical gene therapy gel that has shown remarkable success in accelerating wound healing and reducing pain in patients with dystrophic EB.
Stem Cell and Tissue Engineering Advances
Current research now includes gene-edited skin grafts like Zevaskyn, which aims to correct underlying genetic defects while promoting natural wound healing. Stem cell therapies are being investigated for their potential to regenerate healthy skin tissue and restore normal skin function. These approaches represent a fundamental shift from symptom management toward addressing the root genetic causes of EB.
The Road Toward a Systemic Cure
While current treatments still focus on managing symptoms and preventing complications, researchers and advocacy groups are actively working toward more comprehensive solutions. The long-term goal is developing systemic therapies—ones that address the entire body rather than individual wounds—using gene therapy to correct the underlying protein defects that drive blistering and increase cancer risk.
No Baby Blisters
City: Colorado Springs
Address: 731 Chapel Hills Drive
Website: https://nobabyblisters.org/
Comments
Post a Comment