Epidermolysis Bullosa Genetic Factors and Treatments For Infants & Toddlers
Key Takeaways
- Genetic Root Causes: Epidermolysis Bullosa (EB) is an incurable genetic disease caused by mutations in genes responsible for producing proteins like keratin and collagen, which act as "molecular glue" for the skin.
- Clinical Severity: In its most severe forms, children can suffer with up to 80% of their skin missing at any given time, leading to excruciating pain and life-threatening complications.
- Specific Genetic Classifications: There are four primary types of EB—Simplex, Junctional, Dystrophic, and Kindler Syndrome—each caused by different genetic defects affecting various skin layers.
- Critical Care Requirements: Because the disease is rare and severe, children require specialized non-adherent bandages, severe pain medicine, and high-calorie nutrition to survive.
Reading about the genetic foundation of epidermolysis bullosa (EB) can help parents understand why their children's skin behaves so differently and why traditional treatments often fall short. The answer lies deep within cellular structures that most people never think about - the proteins that hold skin together.
The Biological Foundation of Epidermolysis Bullosa
Epidermolysis Bullosa (EB) is a rare, life-threatening genetic condition characterized by extreme skin fragility. The disease is defined by the body's inability to produce functional structural proteins that act as molecular glue, anchoring the various layers of the skin together. In a healthy individual, a complex network of proteins ensures the epidermis and dermis remain bonded under mechanical stress. For children born with EB, genetic defects disrupt this bond, leading to excruciating pain and the constant formation of blisters from even the slightest friction or pressure.
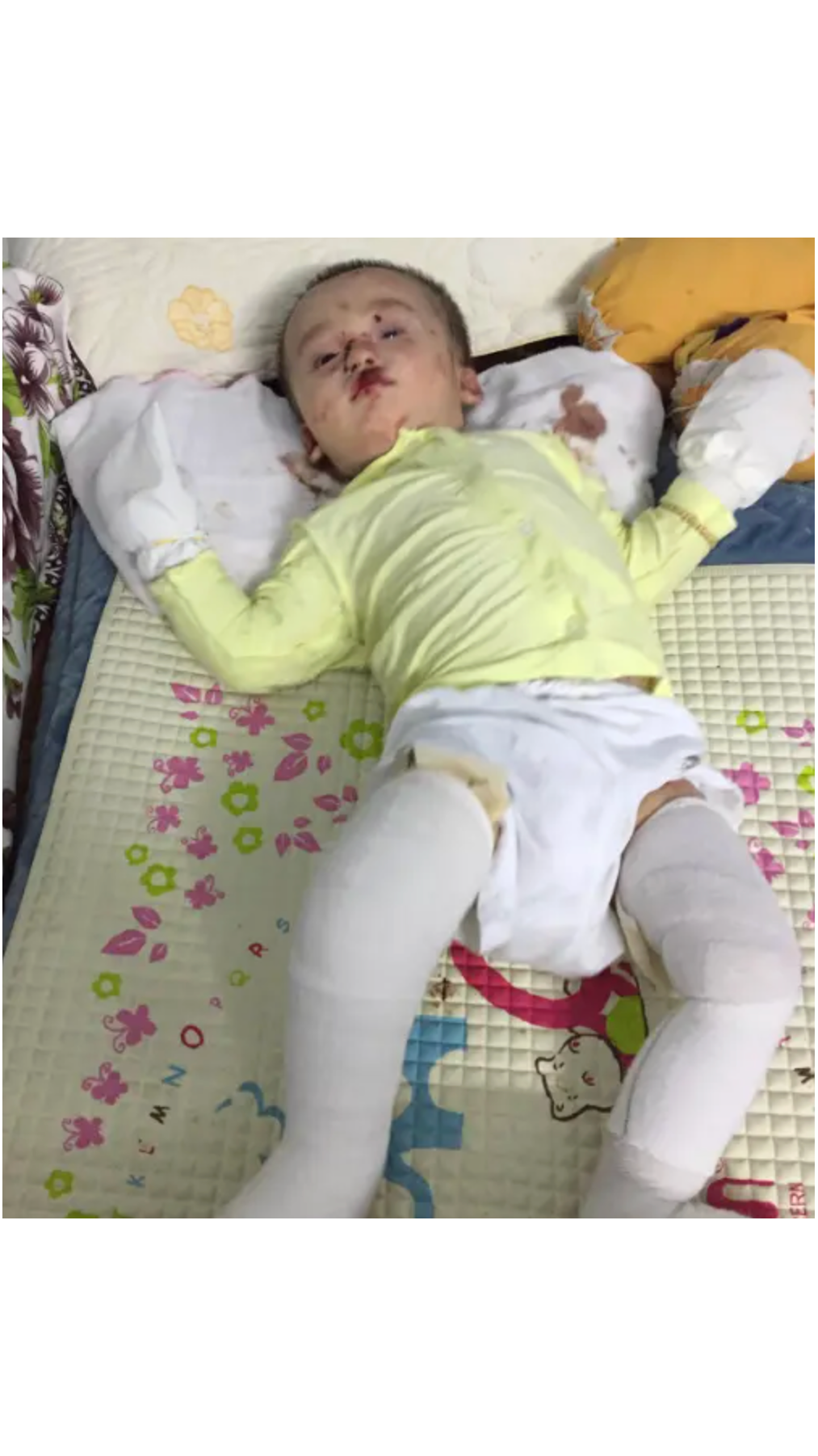
In its most severe clinical presentations, infants can suffer with up to 80% of their skin missing or blistered at any given moment. This level of skin loss is comparable to severe third-degree burns, yet it is a permanent, ongoing state for these children. The clinical reality for these families involves a 24/7 cycle of excruciating wound care, where every touch is a potential injury.
EB Gene Mutations Disrupt Critical Skin Bonding Proteins
The pathology of EB is rooted in mutations within genes responsible for encoding proteins that maintain the dermal-epidermal junction. These proteins, including various types of keratin, laminin, and collagen, are essential for the structural integrity of the skin. When these genes are mutated, the resulting proteins are either absent or severely malformed, leaving the skin architecture in a state of constant collapse.
The dermal-epidermal junction is a specialized basement membrane that separates the outer epidermis from the underlying dermis. Healthy genetic blueprints produce keratin filaments that provide internal strength to skin cells, as well as anchoring fibrils—primarily composed of Type VII collagen—that hook the layers together. For a child with medically neglected EB, these microscopic "hooks" do not exist, making the skin as fragile as a butterfly's wing.
Four Primary Genetic Classifications of EB
Medical literature identifies four distinct types of EB, each categorized by the specific gene mutation and the layer of skin where blistering occurs:
- Keratin Gene Mutations (EB Simplex): Resulting primarily from mutations in the KRT5 or KRT14 genes, this form causes blistering within the epidermis. While sometimes considered less severe, the constant friction on hands and feet leads to chronic discomfort and mobility issues.
- Laminin and Collagen Defects (Junctional EB): This severe form involves mutations in genes such as LAMA3, LAMB3, or LAMC2, which encode the protein laminin-332. Blistering occurs within the basement membrane zone. Infants with this classification often face life-threatening complications, including internal blistering of the mucous membranes.
- Collagen VII Mutations (Dystrophic EB): Caused by defects in the COL7A1 gene, this type prevents the formation of anchoring fibrils. Without these fibrils, the epidermis slides off the dermis, causing deep wounding and severe scarring that can lead to "mitten hand" deformities and secondary health conditions like aggressive skin cancers.
- FERMT1 Mutations (Kindler Syndrome): A rare form that causes blistering across multiple skin layers and is often accompanied by extreme sensitivity to light and progressive skin mottling.
The Life-Threatening Reality of 80% Skin Loss
The genetic disruption of skin bonding transforms minor friction—such as the texture of clothing or a gentle hug—into a medical emergency. For an infant, this means that simple movements can cause the skin to peel away in large sheets. The lack of a protective barrier leads to a constant state of vulnerability.
The complications of such extensive skin loss are manifold:
- Fluid Loss and Malnutrition: Large open wounds lead to the loss of essential fluids and proteins. Children often require specialized high-calorie nutritional support because their bodies expend all available energy attempting to heal massive wounds that never truly close.
- Sepsis and Infection: Open wounds are a gateway for life-threatening infections. Without access to specialized bandages and life-saving antibiotics, the risk of sepsis is constant.
- Internal Manifestations: The same genetic mutations affecting the skin also impact the internal linings of the body. Blistering in the esophagus can lead to strictures, making it impossible for a child to swallow solid food, necessitating the use of feeding tubes.
The Global Crisis of Medical Neglect
While the genetic cause of EB is the same worldwide, the outcome for children is often dictated by their geographic location and financial status. Many children in underserved regions are considered medically neglected, as they lack access to even the most basic wound care supplies. Standard medical gauze is insufficient; it often sticks to the wounds, causing further skin loss when removed.
Providing relief for these children requires specialized, non-adherent bandages that can cost thousands of dollars per month—an expense that is unattainable for families in poverty. The burden on the caregiver is immense, involving hours of daily wound cleaning and bandaging that must be done with surgical precision to prevent further trauma.
Emerging Gene Therapy and the Fast Cure Plan
Research into gene therapy offers a promising path forward by targeting the genetic root of the disease rather than only providing relief for the symptoms. Two primary avenues of research are currently being explored:
- Systemic Gene Therapy: Unlike localized patches that only assist small areas of skin, systemic therapy seeks to deliver corrective genetic material to the entire body. This is a critical distinction, as children with 80% skin loss cannot be helped by localized treatments alone.
- Molecular and Natural Research: Supplemental research is investigating the use of specific molecular compounds and natural ingredients to reduce the chronic inflammation that prevents wounds from healing.
Some organizations involved in EB care fundraising and research are employing a Multi-Pronged approach to accelerating this research. It prioritizes developing solutions that are not only effective but also affordable. This focus on affordability is vital; a potential cure is only successful if it can be reached by the 500,000 sufferers globally, particularly those in impoverished nations.
Urgency: Helping Children Survive Today
While the goal is a potential full-body cure, the immediate focus remains on survival. Children living with 80% skin loss cannot wait for years of research to conclude; they need severe pain medicine, life-saving antibiotics, and clean, specialized bandages today.
Donor involvement is vital to securing the funding necessary to ensure that these supplies never run out. This support allows charities and caregivers to reach children in underserved regions across multiple continents, providing the medical equipment and nutritional support required to keep them stable. Every day that a child receives these specialized supplies is a day they are protected from the excruciating pain that defines this genetic condition.
No Baby Blisters
City: Colorado Springs
Address: 731 Chapel Hills Drive
Website: https://nobabyblisters.org/
Comments
Post a Comment