What Is Butterfly Skin? Symptoms, Types & How Gene Mutations Cause It
Key Takeaways
- Butterfly skin (Epidermolysis Bullosa) is a genetic condition where skin blisters from the slightest touch, affecting approximately 500,000 people worldwide.
- Four main types exist: EB Simplex (most common, surface blistering), Junctional EB (severe internal complications), Dystrophic EB (scarring with cancer risks), and Kindler Syndrome (sun sensitivity).
- Gene mutations cause missing proteins that normally bind skin layers together, with more than 20 different genes involved in various EB types.
- Daily management requires specialized wound care and protective strategies, though new treatments like FDA-approved Vyjuvek gene therapy offer hope for certain types.
- Early diagnosis and expert care teams significantly improve quality of life outcomes for children and families managing this challenging condition.
Butterfly Skin: When Touch Becomes Trauma
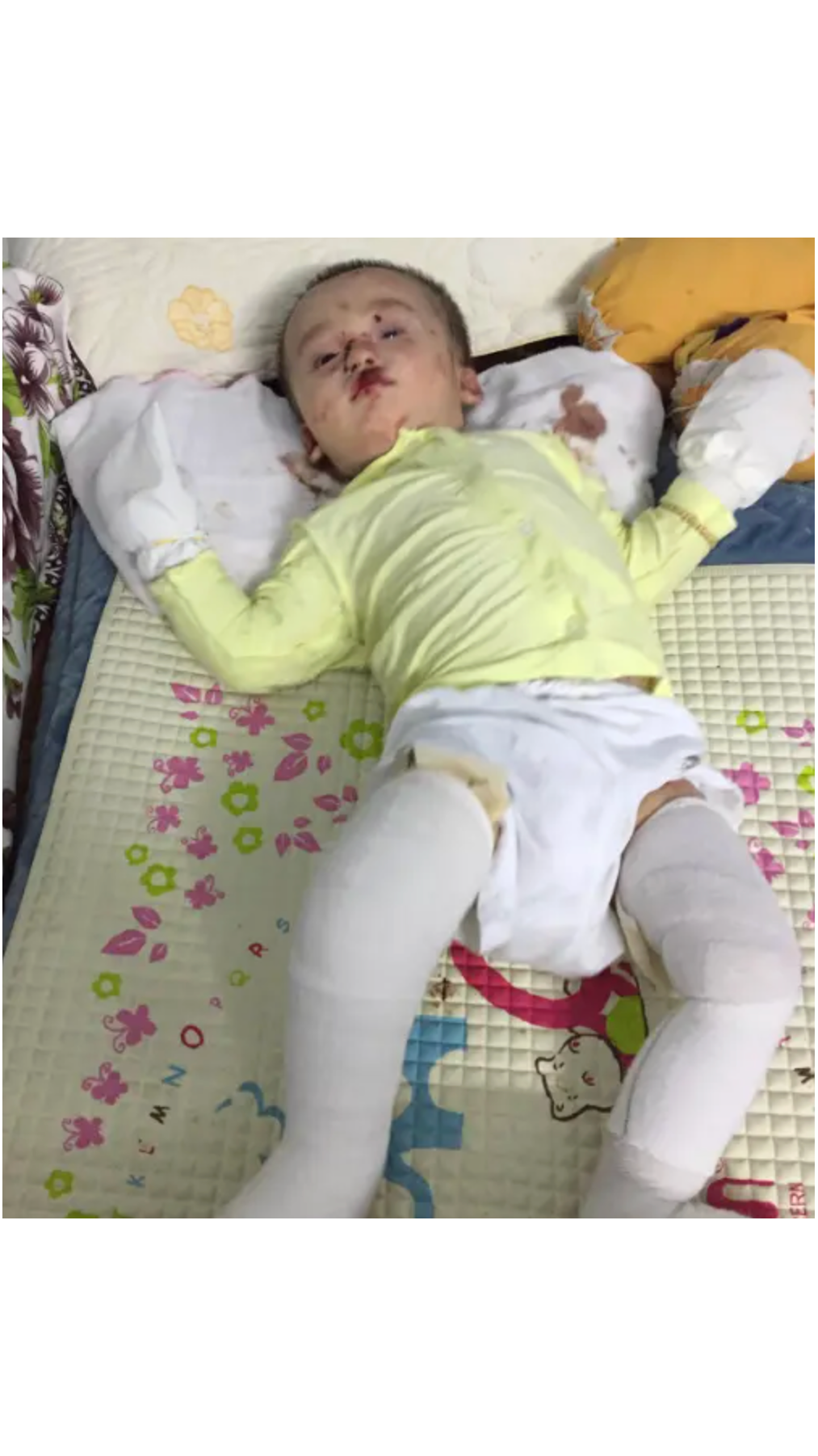
Imagine skin so fragile that a simple hug could cause painful blisters to form. This devastating reality defines life with Epidermolysis Bullosa (EB), a rare genetic condition nicknamed "butterfly skin" because affected skin tears as easily as a butterfly's delicate wings. Children born with EB face a world where everyday activities like getting dressed, eating, or playing become potential sources of injury.
The condition affects approximately 500,000 people worldwide, with an estimated incidence of 20 per million live births. Despite its rarity, the impact on families is profound—transforming simple caregiving tasks into complex medical procedures requiring specialized knowledge and unwavering dedication. Organizations like No Baby Blisters work tirelessly to support families through education, research funding, and advocacy efforts that bring hope to this underserved community.
Understanding EB begins with recognizing that this isn't simply sensitive skin—it's a fundamental structural problem where the proteins responsible for holding skin layers together are either missing or defective. The result is skin that literally falls apart under normal stress, creating wounds that heal slowly and often leave permanent scars.
The Four Types of Epidermolysis Bullosa
EB manifests in four distinct types, each affecting different layers of skin structure. The classification depends on where blistering occurs within the skin's complex layered architecture, from the surface epidermis down to the deeper dermal layers.
1. Epidermolysis Bullosa Simplex (EBS) - Blisters in Surface Skin
EBS represents the most common form of EB, accounting for roughly 70% of all cases. Blistering occurs within the epidermis—the skin's outermost layer—typically triggered by friction or heat. In mild cases, blisters primarily affect hands and feet, often appearing after walking long distances or manual labor. More severe forms cause widespread blistering across the body, including painful oral blisters that complicate eating and speaking.
What distinguishes EBS from other types is that blisters generally heal without scarring, though they may leave temporary discoloration. Many individuals with mild EBS don't receive proper diagnosis until adulthood, as symptoms can be mistaken for severe eczema or other inflammatory skin conditions. The condition often improves with age as skin naturally thickens over time.
2. Junctional EB (JEB) - Severe Form with Internal Complications
JEB affects the basement membrane—a crucial junction zone between the epidermis and dermis. This form typically presents more severe complications, with blisters extending beyond external skin to affect internal mucous membranes lining the mouth, throat, esophagus, and gastrointestinal tract.
The most severe subtype, Herlitz JEB, often proves fatal in infancy due to complications like sepsis, malnutrition, and respiratory failure. Children with JEB frequently experience hair loss from scalp blistering, abnormal nail development, and dental problems including weak tooth enamel. Growth delays are common due to nutritional challenges caused by painful mouth and throat blisters that make eating extremely difficult.
3. Dystrophic EB (DEB) - Scarring Type with Cancer Risk
DEB causes blisters deep within the dermis, resulting in significant scarring that can permanently alter appearance and function. The scarring process often leads to syndactyly—fusion of fingers and toes—creating mitt-like hands that severely impact dexterity and mobility.
Perhaps most concerning, individuals with severe DEB face dramatically increased skin cancer risks, particularly aggressive squamous cell carcinoma that can develop in chronic wound sites. This cancer risk becomes significant during young adulthood, requiring lifelong dermatological surveillance. The condition exists in two inheritance patterns: recessive DEB (more severe) and dominant DEB (typically milder with localized blistering).
4. Kindler Syndrome - Sun Sensitivity and Multi-Layer Damage
The rarest EB type, Kindler Syndrome affects all skin layers simultaneously, creating a unique pattern of symptoms. Beyond typical blistering, individuals experience extreme photosensitivity, requiring constant protection from UV radiation. Skin often develops a characteristic "poikiloderma"—patchy discoloration with visible blood vessels beneath thinned skin.
Only approximately 100 cases have been documented worldwide since 1954, making research and treatment development particularly challenging. The multi-layer damage creates complex wound healing issues, often requiring specialized dermatological and genetic counseling support.
Gene Mutations That Break Skin's Protective Bonds
EB results from mutations in more than 20 different genes, each responsible for producing structural proteins vital for skin integrity. These proteins function like molecular glue, binding skin layers together and providing the tensile strength necessary for normal daily activities.
How Faulty Genes Create Missing Proteins
Each EB type corresponds to defects in specific protein systems. EBS primarily involves mutations in KRT5 and KRT14 genes that produce keratin proteins—the building blocks of the epidermis's structural framework. When these keratins are defective or absent, the uppermost skin layer lacks internal strength, causing cells to rupture under minimal stress.
Junctional EB stems from mutations affecting laminin and collagen XVII proteins, found in the basement membrane zone. Genes like LAMA3, LAMB3, LAMC2, and COL17A1 normally produce proteins that anchor the epidermis to underlying layers. Without these molecular anchors, skin layers separate catastrophically.
Dystrophic EB involves COL7A1 gene mutations that prevent production of type VII collagen—critical for dermal structural integrity. This collagen forms anchoring fibrils that secure the epidermis to the dermis. Its absence allows skin layers to slide apart, creating deep blistering and permanent scarring.
Inheritance Patterns: Dominant vs. Recessive EB
EB follows two primary inheritance patterns or can occur through de novo mutations that determine family risk and disease severity. Dominant inheritance requires only one defective gene copy from either parent, creating a 50% chance of passing EB to each child. Most EBS cases follow this pattern, often with milder symptoms that may not appear until adulthood.
Recessive inheritance requires defective gene copies from both parents, who typically are unaffected "carriers." These couples face a 25% chance of having an affected child with each pregnancy. Recessive forms, including most JEB and severe DEB cases, tend to be more severe since both gene copies are nonfunctional, eliminating any compensatory protein production.
Daily Symptoms Beyond Blistering
While skin blistering defines EB, the condition's impact extends far beyond visible wounds. The complexity of daily symptom management often surprises newly diagnosed families, requiring care strategies that address both physical and emotional challenges.
Pain, Scarring, and Mobility Challenges
Children with EB frequently describe their pain as resembling severe burns, with intensity levels that would incapacitate most adults. The pain isn't limited to active blistering—healed areas often remain hypersensitive, creating ongoing discomfort that affects sleep, mood, and developmental milestones.
Progressive scarring creates functional limitations that compound over time. Contractures—permanent shortening of muscles and tendons around scarred joints—can severely limit range of motion. Many children require adaptive equipment, physical therapy, and sometimes surgical releases to maintain basic mobility. Foot blistering makes walking painful, often necessitating wheelchair use even when muscle strength remains normal.
The psychological impact proves equally challenging. Children may become withdrawn, avoiding physical activities and social interactions that could trigger new blisters. Parents often struggle with protective instincts that conflict with children's developmental needs for exploration and independence.
Internal Complications Affecting Eating and Growth
Internal blistering creates cascading health complications that extend far beyond skin concerns. Esophageal blisters and subsequent scarring can cause strictures—narrowed passages that make swallowing increasingly difficult. Many children require surgical dilation procedures or feeding tubes to maintain adequate nutrition.
Chronic malnutrition becomes a primary concern, particularly in severe EB types. Mouth blisters make chewing painful, while gastrointestinal involvement can impair nutrient absorption. Anemia develops frequently due to chronic blood loss from wounds, protein loss through damaged skin, and nutritional deficiencies affecting red blood cell production.
Growth delays often persist despite aggressive nutritional interventions. The body's energy demands for constant wound healing compete with normal growth requirements, creating a challenging balance for pediatric care teams to manage.
Expert Care Provides Hope for Managing Your Child's EB
While EB remains incurable, specialized care dramatically improves outcomes and quality of life. Modern treatment approaches combine advanced wound management, pain control, nutritional support, and emerging therapies that target the condition's genetic roots.
The FDA's 2023 approval of Vyjuvek (beremagene geperpavec-svdt) represents a breakthrough in EB treatment. This topical gene therapy delivers functional COL7A1 genes directly to skin cells in patients with dystrophic EB, enabling production of normal type VII collagen. Applied weekly by a healthcare professional or trained caregiver, Vyjuvek helps wounds heal faster and reduces new blister formation.
Care for EB requires multidisciplinary teams including dermatologists, wound specialists, nutritionists, pain management experts, and mental health professionals. Daily wound care protocols, specialized dressings, and protective strategies form the foundation of management, while emerging treatments offer hope for more definitive solutions.
Research continues advancing on multiple fronts, including stem cell therapies, protein replacement treatments, and additional gene therapy approaches. Clinical trials provide access to treatments while contributing to the scientific understanding that will benefit future generations.
No Baby Blisters
City: Colorado Springs
Address: 731 Chapel Hills Drive
Website: https://nobabyblisters.org/
Comments
Post a Comment